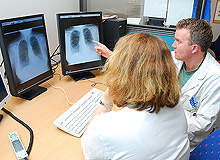
Political restrictions, distance and other stumbling blocks such as language and data barriers have traditionally restricted international collaboration between hospitals. With the advancements in digital technologies and the general trend of globalisation pervading all major industry sectors, however, hospitals and healthcare providers are now finding it easier than ever to reach out beyond their home markets.
Supported by numerous initiatives and programmes such as the UK’s ‘The International Health Links’ by the Tropical Health and Education Trust (THET), cooperation between hospitals has experienced a boost worldwide. The programme promotes links or partnerships between health care organisation in the UK and a developing country with the purpose to bring people working together "to share ideas, knowledge and friendship to improve healthcare."
The World Health Organization (WHO) and the International Hospital Federation (IHF) also support international partnerships and actively promote collaboration. In February 2011, the two authorities published a draft of the paper ‘Hospitals’ challenges and WHO portfolio of hospital related activities: Exploring the way forward’, with particular focus on the international collaboration of hospitals.
According to the report, similar challenges can be found in hospitals all over the world, even though the sector is organised differently from one country to another. A global generic hospital model and international collaboration on all levels could overcome the challenges, which are especially related to hospital environment, hospital inputs, operations, functions and output.
Cooperation on all levels
Collaboration between hospitals can take place on different dimensions and levels. Institute-to-institute collaboration from one hospital to the next is the most common form of cooperation. However, collaboration also takes place from one department to the next or from one individual doctor to another.
See Also:
University of Michigan Medical Innovation Centre (MIC) fellow and hospital management consulting firm BPL International associate, Hannah Hensel, explains: "We’ve found that there are different dimensions of collaboration."
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataThe company focuses on market growth strategies for healthcare providers, medical device and medical technology companies in emerging markets. The president Robert H. Barrow says: "Hospital and healthcare in broader terms are in different stages of development, particularly if you look at providers in the US and Europe, which are very mature markets from their healthcare point of view, compared to China and India."
"If we look at some of the rapidly developing countries, there is a huge demand for healthcare. Demand is growing extremely quickly because the population is growing with that also the money and ability to pay for healthcare services," he says.
India, for instance, will double its ability to pay for healthcare from 2008 to 2014, with currently 260 million people in the mid and upper income demographical group of the total population of 1.1 billion. The country has also started moving towards a life-style burden of disease (BoD). "Cardiac, diabetes and cancer rates are significantly increasing and one of the highest BoD in that country," says Barrow.
"The other thing indicating the growth is that in India around 800 new hospitals are required over the next ten years just to meet demand. That’s really a massive growth," he continues.
Shift towards emerging markets
Barrow thinks that the increasing demand makes collaboration between hospitals important – especially between highly qualified hospitals in Europe or the US and providers in emerging countries. Assisting new collaborations with the strategic planning process, the implementation and start-up phase and the operational performance improvement are the main purpose of BPL International’s work.
According to Robert H. Barrow and Hannah Hensel, there has been a shift in the international collaboration from the Middle East and the Gulf States in the past 15-20 years towards emerging markets in Asia, parallel with a shift towards middle-income patients instead of "extremely wealthy people" in the Middle East.
"What we are seeing now is more of an emerging market strategy with growth in the middle-income groups in Asia particularly," says Barrow. The benefits for those countries are obvious as they try to improve the quality of their healthcare service, the clinical excellence as well as the number of their beds and service lines.
"Particularly in China and certainly India, the reputation of the European and US healthcare providers is very important," says Barrow. "We’ve seen examples where hospitals are looking to develop around a certain service, such as neurology or orthopaedics, and they want to collaborate with a US or European hospital because of their very high degree of quality of care and technology." Other areas of collaboration can include research, testing and education of medical staff.
Western hospitals, however, have to be careful when they move into emerging markets to broaden their value and branding globally. "The US and even the UK have a highly regulated health care industry and if they move into potentially emerging markets, which are not regulated they have to be very cautious and careful on ensuring the collaboration works properly on both sides," explains Barrow.
"US healthcare providers want to be able to say that they are a global provider and that they have patients and operations from overseas," continues Barrow. "I think it’s for two reasons: it is good business but they also genuinely believe it’s an opportunity to help raise the overall quality of healthcare in that country."
Sharing expertise, know-how and state-of-the-art technology can then help raise the overall quality of care for patients in those countries.
Telemedicine
Different types of collaboration have the use of new communication and information technologies in common, which facilitate work and operational processes. Especially the field of telemedicine – or medicine that is remotely administered – has been associated with successful collaboration throughout the past 20 years. Today, telemedicine is making a comeback as part of international collaborations to overcome challenges such as the increasing ageing of the world population and the growing lack of qualified personnel in certain branches of professional healthcare.
The Norwegian Centre for Integrated Care and Telemedicine head of advisory department Line Linstad believes that the opportunities of telemedicine have not been realised yet. "In Europe it’s not being done on a very large scale yet, although on a hospital macro-level it would be very useful, especially for smaller and emerging countries."
"On a technology level we have a lot of quite mature technologies, which can be tailored to underpin the needs of clinics," she explains. "But first hospitals have to overcome organisational, institutional and regulatory challenges to use telemedicine for successful cooperation between hospitals across borders."
According to Linstad, hospitals will first have to change the way they are working, which needs strong leadership and a foolproof strategy. Regulatory restrictions are another issue, in particular when it comes to security of the patient information and the licensing of practitioners across borders for international cooperation.
Telemedicine laws vary from US state to US state, and also European countries have separate national regulations. In addition to that, the EU adopted a directive for patient’s rights in cross-border healthcare in January 2011. Proposed by the European Commission in 2009, the step came after the member states themselves called for European-based legislation on telemedicine to clarify cross-border healthcare and the use of new technologies.
"With the population getting older and the change in demographics we need to find tools to make the things we are doing more cost-effective," says Linstad. "Hospitals can use these new technologies to work in a more gainful way. Telemedicine can be used to realise the international goals and strategies of hospitals and it is management responsibility to work for realising the potential that comes with telemedicine."
Linstad believes that the whole potential of the technologies has not been realised yet. "Neither for cross-country collaboration nor for collaboration within a country like Norway," she says. "We are just at the beginning."
Also BPL International has recognised the need for even better technology to make international collaboration easier. "We’re working on developing a technological solution that is able to facilitate international collaboration, the exchange of data against the physical appearance of the patient and then the interaction between the two," says Hannah Hensel.
But what is foremost to successful collaboration is that both parties benefit from the cooperation. "The main challenge is determining the value proposition for both partners that wish to collaborate and to ensure that the collaboration really adds value to both parties in the long term," says Robert H. Barrow. Then international collaboration between hospitals and other medical facilities can be successful in the long run.
"It’s just exciting how this phenomenon has happened, working together to improve health care," says Hannah Hensel. "And yes a motivator certainly is from a business standpoint but ultimately this motivation is a benefit to society."







