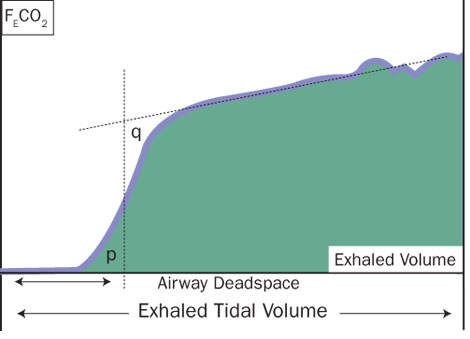
Volumetric capnography is the combination of mainstream CO2 and airway flow measurements. It provides a quantitative assessment of the net quantity of CO2 exhaled (VCO2) on a breath-by-breath basis. Carbon dioxide elimination is affected by ventilation, circulation/perfusion and, to a much lesser degree, diffusion.
Monitoring VCO2 provides a valuable marker for describing the patient’s current cardiorespiratory status and, more importantly, assessing changes in the status of a ventilated patient over time.
CLINICAL APPLICATIONS
Changes in ventilation and perfusion rapidly affect VCO2. Carbon dioxide exhaled in steady state conditions reflects the total CO2 production (that is, metabolism) in the body. Several factors may lead to an increase or decrease in VCO2. Carbon dioxide exhaled changes in concordance with a patient’s physical activity level. It decreases when the patient is asleep or sedated and increases when the patient has a fever or is shivering. These are examples of changes in VCO2 secondary to a change in the patient’s metabolic rate.
On the other hand, changes in ventilator settings or other similar clinical interventions can also change ventilation and perfusion relationships, and thus result in a VCO2 change. For example, a decrease in VCO2 after a change in PEEP may indicate an increase in ventilation-perfusion mismatch secondary to atelectasis, assuming there are no other concurrent changes in the status of the patient.
See Also:
When a decrease in ventilation or circulation causes a reduction in VCO2 the reduction is usually transient. The arterial concentration of CO2 will rise until equilibrium is reached, typically in five to 20 minutes depending on the body’s CO2 stores. At some point during the equilibrium, VCO2 will begin to return to its original value.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataObserving changes in the volumetric capnogram while making ventilator changes provides direct feedback of the patient’s gas exchange on a breath-by-breath basis in response to ventilator settings. Volumetric capnography may prove to be a valuable tool when attempting to wean a patient off mechanical ventilation.
PHYSIOLOGICAL DEADSPACE RATIO
Another important application of VCO2 monitoring in the ICU is the determination of physiological deadspace ratio (Vd/Vt). Pulmonary deadspace (Vd) is the component of ventilation that is wasted, as it does not participate in gas exchange. An increase in deadspace represents an impaired ability to excrete CO2.
The normal Vd/Vt is 0.25–0.40. Increased deadspace fraction is a feature of the early phase of acute respiratory distress syndrome (ARDS). Elevated values are associated with an increased risk of death. Study results show that a Vd/Vt>0.5 reliably predicts successful extubation in infants and children.
Measurement of Vd/Vt helps the clinician to understand what is happening at the alveolar-capillary interface and provides an indicator of the effectiveness of ventilation. A Vd/Vt baseline should be established at the onset and then trended throughout the course of mechanical ventilation.
Determination of appropriate PEEP levels is essential for optimal management of the mechanically ventilated patient in the ICU with acute lung injury or ARDS. Maintaining appropriate PEEP levels may prevent lung derecruitment and the development of atelectasis. Excessive PEEP, on the other hand, may further exacerbate the presence of over-distension and adversely affect cardiac performance.
Optimisation of PEEP can be effectively achieved by monitoring VCO2 and the slopes of the different phases of the volumetric capnogram. Excessive PEEP levels lead to a decrease in VCO2 and the slope of the phase II in the volumetric capnogram.
PULMONARY EMBOLISM
Monitoring of VCO2 has also found applications in the detection of pulmonary embolism. In the ICU, objective testing for pulmonary embolism is crucial, since clinical assessment alone is unreliable and the consequences of misdiagnosis are serious.
Exploiting differences in the shapes of the volumetric capnogram, especially the slope of phase III, holds promise for the early bedside non-invasive determination of pulmonary embolism. More recently, monitoring VCO2 has also been shown to be useful in the assessment of pulmonary perfusion and non-invasive determination of cardiac output.
Based on partial CO2 rebreathing differential Fick technique, changes in VCO2 with the addition of a serial airway deadspace for short duration have been used for the development of a non-invasive and automated technique for measurement of pulmonary capillary blood flow and cardiac output.
Monitoring of VCO2 provides the clinician with a valuable tool in the ICU for assessment and monitoring of ventilation, determination of physiological deadspace (Vd/Vt), optimisation of PEEP, screening for pulmonary embolism, assessment of pulmonary perfusion, and non-invasive determination of cardiac output.