The current 2017–2018 influenza season is rivalling the historical H1N1 pandemic of 2009–2010, which caused a global death toll at more than 284,000 people.
By tracking the Center for Disease Control’s (CDC’s) weekly flu map, the number of states in the US that have widespread influenza activity increased from just three on 25 November 2017, to 35 on 23 December, to 48 by 27 January, the latest week with available data. Within the US, Texas has the highest flu activity according to Walgreen’s Flu Index, which compiles prescription data for antiviral medications used to treat influenza to determine areas with highest incidence of flu.
Numerous factors contribute to the spread of influenza; however, the GlobalData Epidemiology team believes that factors such as low vaccine uptake rate and multiple circulating strains may contribute to why Texas is more susceptible to the spread of the flu.
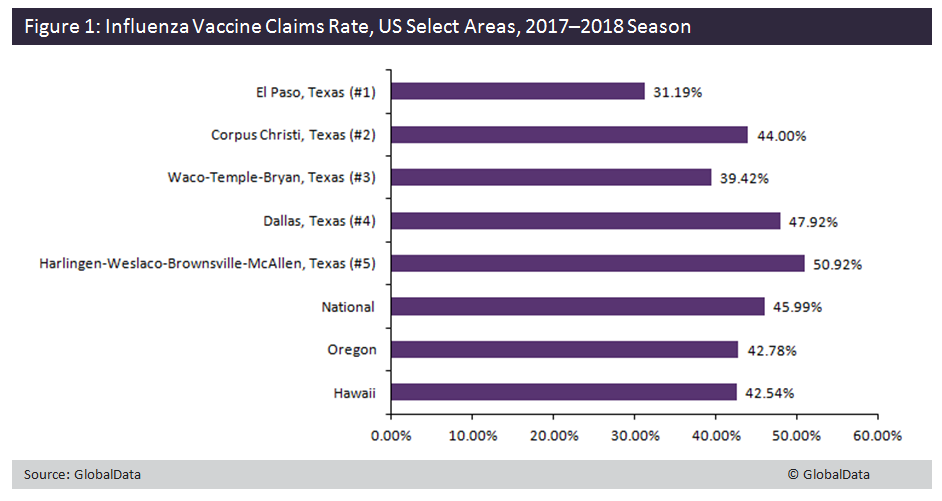
The Walgreen’s Flu Index reported the top 10 US market areas with flu activity, seven of which are in Texas. GlobalData examined the influenza vaccination rates of the top five market areas with flu activity, as well as Oregon and Hawaii, the two states currently with lowest flu transmission levels in the country. Influenza vaccination rates were obtained through the US Department of Human Health Services’ statistical database on vaccination claims among Medicare beneficiaries for these areas in the US.
This vaccination rate should not be interpreted as the total influenza vaccine uptake for the US, since the Medicare population is not representative of all populations in the country. However, it can be used to compare vaccination rates across regions. In the figure below, it’s shown that the first and third-ranked flu activity areas have lower vaccination rates compared with the national rate. However, other areas in Texas have vaccination rates similar to the national rate, some even higher.
See Also:
Vaccination rate alone cannot explain high transmission rates in Texas. GlobalData also examined the characteristics of positive influenza tests reported to the CDC using the FluView database. We found that Texas reports less predominance of the main strain than the national level, and more strains than the states with lower transmission.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalData
In Texas, six strains were reported, with the most common being type A(H3), at 59%. In the US as a whole, 76% of those tested were A(H3) strain. Oregon reports 3 strains only, while Hawaii also reports about 76% of the positive tests being A(H3). We believe Texas may be experiencing lower community immunity due to low vaccination rates, low effectiveness of this season’s vaccine, and the multiple strains in transmission, factors that contributed to it being a high area of flu transmission.
GlobalData’s PharmaPoint: Seasonal Influenza Vaccines – Global Drug Forecast and Market Analysis to 2025 report had identified a higher level of public awareness and positive perception of influenza vaccines, as well as vaccines with broader strain coverage, as key opportunities in the seasonal influenza market. Although this year’s vaccine does not have high levels of protectiveness against the flu, it does offer some protection and will decrease disease severity. Future developments of vaccines that address these unmet need areas would be beneficial for high flu activity areas such as Texas.








Related Company Profiles
CDC SpA
Medicare Corp.