Diabetic ulcers heal more easily if they are kept moist but not macerated, and are protected from contamination. BSN Medical’s Cutimed Siltec dressing meets all these requirements.
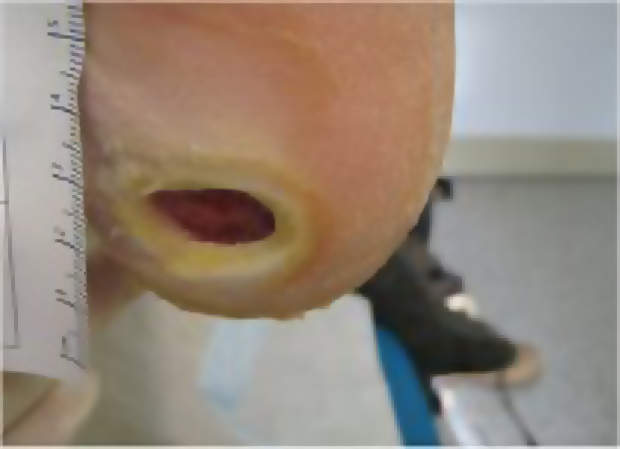
A 58-year-old man was admitted to hospital with a wound on his left heel. A full clinical assessment was carried out which revealed the patient, a smoker, was a non-insulin dependent diabetic with associated polyneuropathy. The ulcer, on the plantar surface of his left heel, was about 1.5cm in diameter and had been there for around three months. It produced a moderate amount of exudate although it was relatively free from odour.
Diagnosis and treatment
The patient was prescribed Metformin, to be taken twice daily, for control of his diabetes, and a structured programme for the management of his wound was initiated. This began with intensive surgical debridement of the wound bed and the surrounding skin to remove callus built up around the wound margin, (Figure 1).
The wound was irrigated with Lavasept, a solution containing 0.2% polyhexanide, an antimicrobial agent with a broad spectrum of activity, and dressed with Cutimed Siltec to protect it from contamination while providing a moist wound-healing environment. In the initial treatment stages, the wound was subject to wet to dry cleansing.
The importance of offloading, relieving or eliminating pressure on the affected area was explained to the patient and achieved both by elevating the limb and using orthopaedic braces as appropriate.
The patient remained in hospital for two weeks, after which time he was managed as an outpatient in the hospital’s day clinic. During this time, dressing changes were typically carried out every four days.
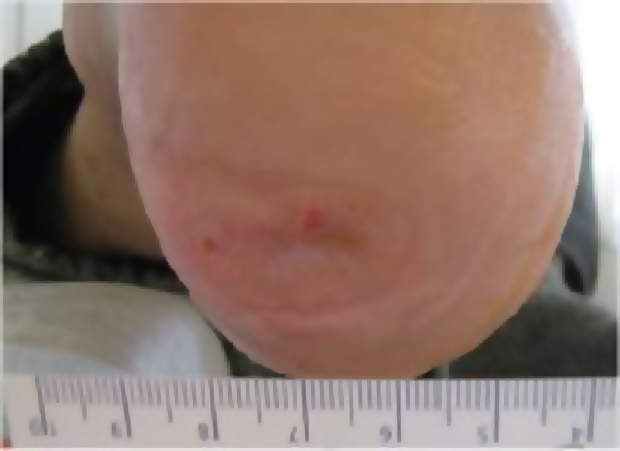
Changes five to seven were performed by the patient himself, a procedure he reported easy and pain-free. After less than two weeks, an improvement was clearly visible, (Figure 2) and after one month the lesion had reduced to around 0.3cm in diameter (Figure 3).
Further improvements were noted at successive dressing changes and as a result the wound healed in approximately four weeks with no complications, although the patient was told to continue to employ the offloading techniques for a further three months. At the end of this time, he was given custom-made orthopaedic footwear to prevent a reoccurrence of the pressure damage and was invited to attend clinic on a six-monthly basis for follow-up inspections.
Minor injury source
Diabetic neuropathy is a common source of minor skin injury associated with pressure or friction caused by ill-fitting shoes, or an undetected foreign body such as a small stone in a shoe. If left untreated, these types of wounds can rapidly extend or form ulcers which, if they get infected, can have serious consequences. Unlike wounds caused by peripheral vascular disease, which are also common in diabetic patients, neuropathic ulcers heal a lot more easily providing they are managed in the right way.
Initial treatment involves removing the source of pressure. This is often achieved by wearing the right shoes, and a period of offloading which will enable the tissue to recover. Appropriate local wound management is also important and this may involve using systemic antibiotics where indicated, or applying a dressing that has some inherent antimicrobial activity.
For non-infected wounds, an appropriate dressing may be all that is required, one able to provide the optimal conditions for healing by keeping the wound moist but not macerated, and providing a physical barrier to external contamination. For diabetics, like other patients who may have fragile or easily-damaged skin, it is important the dressing chosen does not cause trauma on removal or produce maceration of the periwound skin as it could lead to further damage.
The Cutimed Siltec dressing met all requirements and provided the ideal treatment. It was easy to use and its transparency allowed the wound’s condition between dressing changes to be monitored, an important factor if a dressing is to be left untouched for several days.