Data have shown that the prevalence rate of major depressive episodes (MDEs) in adolescents is steadily increasing in the US. A major depressive episode is defined as a period of two weeks or longer during which there is either depressed mood or loss of interest or pleasure, and at least four other symptoms that reflect a change in functioning (such as problems with sleep, eating, energy, concentration, self-image, or recurrent thoughts of death or suicide), as described by the fourth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV). The difference between an MDE and a major depressive disorder (MDD) is that MDEs include depressive episodes that occur as part of bipolar disorder, while MDD does not include bipolar depression. However, when examining MDEs and MDDs, the majority of lifetime MDE is MDD.
The US National Survey on Drug Use and Health (NSDUH) reports that the 12-month prevalence of MDEs in adolescents increased from 8.7% in 2005 to 11.3% in 2014, and 12.8% in 2016. Female adolescents were approximately three times as likely to have a major depressive episode, compared to males, at 19.4% and 6.4%, respectively.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
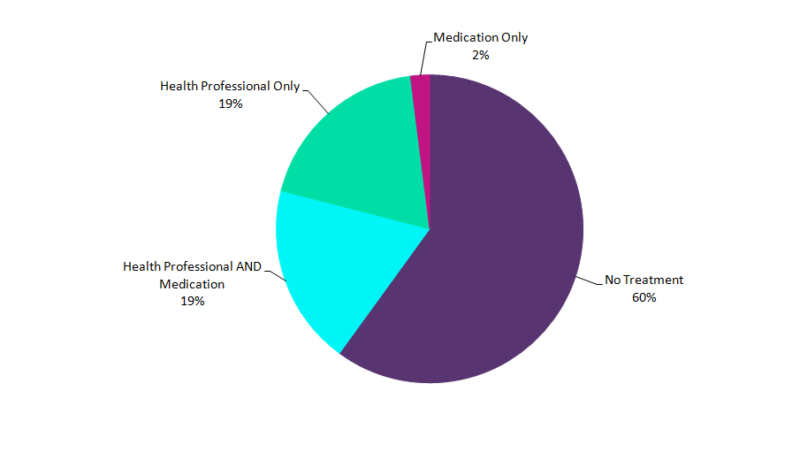
By GlobalDataFigure 1: Treatment received among adolescents with major depressive episodes within the past year, both sexes, ages 12–17, 2016

Source: GlobalData; Substance Abuse and Mental Health Services Administration
See Also:
Figure 1 shows that in 2016, approximately 60% of adolescents with MDEs reported that they did not receive treatment (treatment types included health professional only, medication only, and combined health professional and medication), according to the National Institute of Mental Health and the Substance Abuse and Mental Health Services Administration.
There are many consequences associated with not treating depression, including emotional, behaviour, and health problems. Epidemiological studies have examined the adverse effects of mental disorders on four main areas: education, marital timing and stability, childbearing, and education. Economic costs associated with behavioural health disorders have reached up to tens of billions of dollars annually, which includes healthcare costs and lost productivity, according to the Alliance of Community Health Plans. Depression is treatable, but the illness must first be recognized for it to be treated.
Related reports
GlobalData (2016). EpiCast Report: Major Depressive Disorder – Epidemiology Forecast to 2025, October 2016, GDHCER125-16









Related Company Profiles
DSM IV BV
MD&E, Inc.