Patients may still think, or at least wish, their doctors to be infallible. But, much as they may not care to admit it, most clinicians know and accept that, deep down, they can make mistakes just as easily as the next person, particularly if they are over-worked, under pressure or exhausted at the end of a long shift.
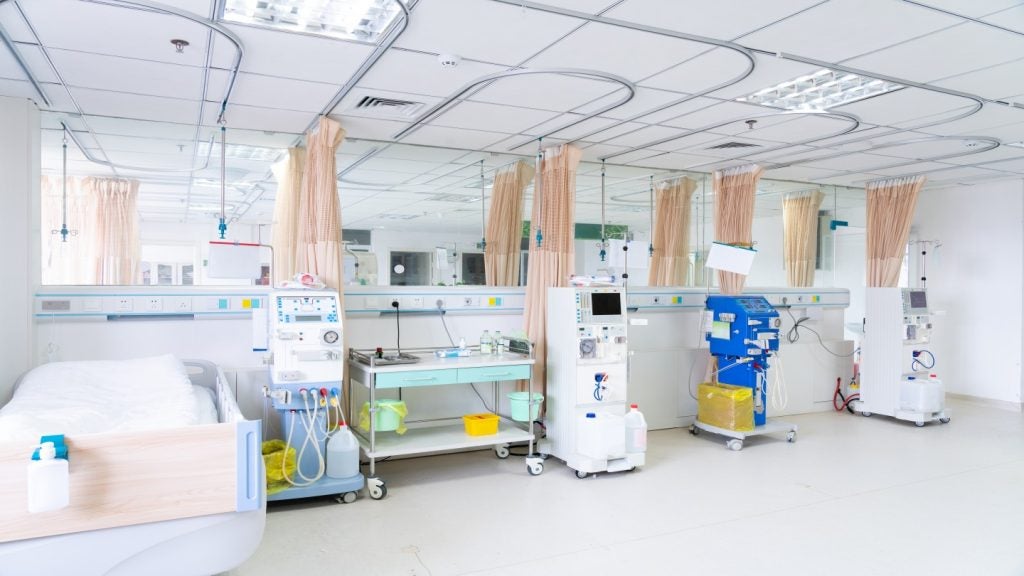
The hope is, of course, that such mistakes will be rare and inconsequential in the wider scheme of things. The sad reality, however, according to latest research, is that mistakes in the administration of injected medication within the intensive care unit (ICU) environment in particular, occur far more frequently than administrators, clinicians and certainly patients should expect, and are a serious safety problem that needs to be addressed by staff at all levels within ICUs.
Safety at stake
The study, published online in the British Medical Journal in March 2009, concluded that injected medication errors were “a serious safety problem” within ICUs and occurred “with alarming frequency”.
The research, led by Dr Andreas Valentin of the General and Medical Intensive Care Unit at Vienna’s Rudolfstiftung Hospital, followed a previous study that had found medication errors were frequent at the administration stage within the ICU setting and intended to look at this issue at the multinational level.
The research team monitored errors occurring at 113 ICUs in 27 countries over the same 24-hour period, from 17-24 January 2007. All nurses and physicians on duty during the study period were asked to record errors using a questionnaire available at the bedside of each patient.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataErrors were categorised by type of error, type of drug administration and class of drug and a detailed description of the error was recorded to allow assessment of contributing factors. Further data were recorded to calculate occupancy rate, relative turnover, patient-nurse ratio, and patient-to-physician ratio for each shift in the ICU. The severity of illness in each patient and nursing workload were also assessed on the day of the study.
Study results
What Valentin and his team found from their research was that, in a total of 1,328 patients, 861 errors affecting 441 patients were reported over the 24-hour period. Just over two thirds (67%) of patients experienced no error, 250 patients (19%) experienced only one error and 191 patients (14%) experienced more than one error. Although 71% of the errors resulted in no change in the status of the patient, 12 patients (0.9% of the total study population) suffered permanent harm or death related to a total of 15 medication errors that occurred at the administration stage. Trainees were reported as being involved in eight of these errors.
The most frequent mistakes related to wrong time of administration (386) and missed medication (259), followed by wrong dose (118), wrong drug (61), and wrong route (37). Workload / stress / fatigue was reported by ICU staff as a contributing factor in 32% of all errors. Other contributing factors included a recently changed drug name (18%), communication – written (14%), communication – oral (10%) and violation of standard protocol (9%).
The odds for the occurrence of at least one medication error increased significantly with a higher severity of illness, a higher level of care, and a higher rate of parenteral drug administrations. This finding directly reflected the complexity of care of these patients and thus the increased opportunity for error, the study argued.
By contrast, the odds decreased when a critical incident reporting system was in place and when there was an established routine of checks at nurses’ shift change. Mistakes commonly occurred with the administration of insulin for diabetics, sedatives and blood-clotting drugs. Just one in five units reported no adverse events during the 24-hour period studied.
A new approach
This study concluded that the administration of parenteral medication was a weak point in patient safety in the ICUs.
Worryingly, since the results were based on data from 113 participating ICUs worldwide, this was a problem that represented a common pattern.
The increasing complexity of care in critically ill patients meant that organisational factors such as error-reporting systems and routine checks at shift changes were needed to reduce risk of errors in ICUs.
“We need a new approach where it is acceptable to recognise and accept that errors will sometimes happen. You can never have an absolutely perfect system, but you can perhaps get closer to one. It is about raising awareness of the situation and analysing it in a detailed way,” stresses Valentin.
“There are in most cases systemic factors that contribute to the risk that will occur,” he adds.
Time for bed
Fatigue is clearly a major contributory factor, as a similar study in JAMA, the Journal of the American Medical Association, reported in September 2005. It argued that many resident doctors were so sleep-starved that they were effectively “drunk” with fatigue and were therefore unproductive, inefficient and a danger to patients and themselves. Nurses, too, typically worked eight to 12-hour shifts, with some working even longer hours. This meant that, while nurses were technically in a prime position to prevent and intercept mistakes before they were made, they often failed to do so because they were themselves overwhelmed and tired.
Addressing the problem
What’s the answer? Valentin points to a range of relatively simple and cheap ergonomic solutions, such as redesigning or rethinking medication labelling systems, colour-coding and redesigning the typeface to assist tired doctors and nurses in comprehending what they are. Communication and education can be better used too.
More widely, however, hospitals probably need to be looking at issues around manpower, staffing and shift patterns. This could mean the need to redesign shift patterns or ensure that they are being better designed around the natural rhythms of the body to eliminate fatigue.
“A lot of the time it is to do with personal situations which health workers face in their work, such as increased stress, workload and fatigue. If someone is on-shift for 24 or 36 hours, this is clearly not the best way to manage shift rotas. You simply do not react in the same way if you have been working for 24 hours. It affects you in the much the same way as if you were drunk,” agrees Valentin.
“Policymakers and business managers should know this comes at a price. There is no safety without a price,” he adds.
Yet some findings within the research were surprising and the opposite of what you might expect. “We found, for example, that when the ICU staff were in charge of preparing the medication for an infusion, the risk decreased considerably, which is in some ways surprising. You might assume that having this done in the pharmacy, where staff are likely to be working shorter hours and be under less pressure, would be better in terms of risk,” says Valentin.
“But what this shows is that increasing complexity, such as having a process outsourced away from the final provider, can be a factor in risk. It might, in fact, be better to have the final provider, in this case the ICU staff, staying in charge of the process and of the care within the unit. Success is often about gaining or keeping control,” he adds.
Making improvements
Ultimately, the key to unlocking this issue is cultural change; getting to the point where there is recognition that coming forward and reporting (and learning from) errors is not something to be ashamed of or to be stigmatised and, in fact, in the longer term it can be a positive step towards changing the system and reducing the risk of error.
“It could be beneficial to show that reporting errors is actually a good thing. It will often be a question of supervising and managing this correctly and about how you can go about creating a safer environment,” advises Valentin.
“This system can reduce the risk of error but there has to be open discussion about how you are going to get there and then you have to analyse it. You need to look at your statistics and at your every process. It may just be something as simple as checking the rota or changing the shift pattern. But you do need to be looking at your processes in a different way.”